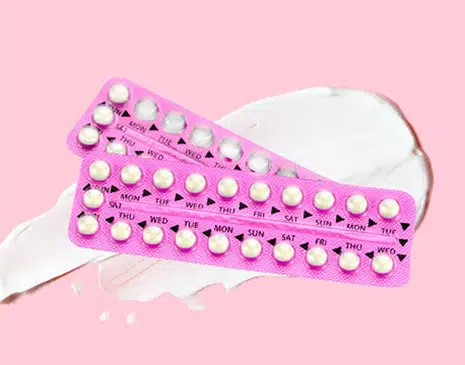
The hormonal birth control – yeast infection connection
The contraceptive pill is often prescribed to prevent unplanned pregnancies and treat a host of other women’s health conditions. The pill is the most convenient and accessible form of birth control available to most women, with a success rate to impress anyone’s plans for a child-free future (until you’re ready to start a fam, that is).
Like all good things, the ease and convenience of religiously popping a pill once a day can cause contrasting side effects, like nausea, headaches, and mood changes. But is it possible that women on hormonal birth control are more susceptible to vaginal yeast infections, like thrush and BV, as a side effect of birth control?
You know we’ve done the research, so let’s find out!
What is a yeast infection?
A vaginal yeast infection, or vaginal candidiasis, is a fungal infection caused by a Candida yeast overgrowth in the body. Symptoms range from vaginal itching, swelling and redness to a thick, creamy-white vaginal discharge. The exact prevalence of thrush is not readily available as it is often under-reported and underdiagnosed. However, it is estimated that up to 75% of women will experience a vaginal yeast infection at some point in their lives, with thrush being one of the most common forms of yeast infection.
Is thrush contagious? Or can thrush be passed on through sex? Well, although yeast infections aren’t considered sexually transmitted infections (STIs), small amounts of bacteria can transmit during sex, throwing the vaginal flora off kilter. So, it is recommended that you avoid kissing, sexual intercourse, and other sexual activity like oral sex when managing vaginal infections.
What are the symptoms of a yeast infection?
Yeast infections are often mild or asymptomatic (another great reason to stay up to date with your STI testing). But when a yeast infection does cause symptoms, they can be annoying as hell to endure.
The most typical symptom of a yeast infection is abnormal vaginal discharge. Some women may experience a chunky, cottage cheese-like substance in their knickers. Others may experience a mild, watery discharge. Both types of abnormal vaginal discharge are usually odourless and accompanied by other symptoms that affect the vulva and vagina areas.
Common symptoms to look and feel out for include intense vaginal itching and inflammation of the vulva, particularly the labia. A painful, burning sensation may also be felt when peeing or trying to have sexual intercourse.
* We used the term ‘trying’ because the pain and discomfort caused by a yeast infection can be so extreme in some cases that reaching orgasm may not be a possibility. And that’s okay; remember your comfort during sexual activity is always a priority.
Here’s a timely refresher on the facts surrounding consent.
What causes yeast infections?
Vaginal yeast infections are caused by a type of yeast called Candida albicans. This type of yeast is part of the body’s natural microflora. It lives in the mucus membranes of the eyes, ears, mouth, gastrointestinal tract, and vagina.
The body is completely happy to host Candida rent-free in exchange for its ability to recognise and destroy harmful bacteria. But, when Candida multiplies and grows in excessive amounts, it can lead to inflammation that disrupts the natural vaginal microbiome and vaginal pH.
Common risk factors and habits that can cause yeast infections include:
- Having a weakened immune system
- Taking antibiotics
- Being pregnant
- Hormonal fluctuations
- Sexual activity
- Having a high-sugar diet or uncontrolled diabetes (yeast thrives in high-sugar environments)
- Wearing sweaty gym clothing for hours post-exercise
- Regularly wearing tight underwear
- Using soaps and products that interfere with natural vaginal flora (aim for natural soaps, and brush up on how to clean your vulva)
- Overusing pads, panty liners, or tampons
Who gets vaginal yeast infections?
Women who have an increased risk of contracting a yeast infection include those who:
- Are pregnant
- Have diabetes
- Have a weakened immune system (due to medications or infections)
- Have recently taken or are currently taking antibiotics
- Use a hormonal birth control method, like birth control pills
So, how does birth control increase the risk of yeast infection?
Two words: Vaginal Microbiome.
The vaginal microbiome (aka the vagina’s natural environment) is influenced by billions of different bacteria, the most important being the healthy bacteria called lactobacilli. Both thrush and bacterial vaginosis are caused by an imbalance of lactobacilli and an overgrowth of Candida in the vaginal canal.
Many forms of hormonal birth control contain a combination of estrogen and progestin that disrupts the body’s natural hormonal balance. This can lead to a higher risk of developing a yeast infection.
To be crystal clear, birth control doesn’t directly cause the common women’s health condition of yeast infection. Rather, oral contraceptives change the environment of the vagina into a space that’s incredibly appealing for yeast to grow, multiply and flourish.
How to prevent frequent or recurrent yeast infections?
Whether you’re on hormonal contraception or sitting in the higher risk bracket for yeast infections, the best way to prevent most yeast infections (and other vaginal infections) is by looking after your vaginal microbiome.
To keep your vagina happy and healthy:
- Avoid unnecessary prescription medication and antibiotics
- Practice safe sex (always use a form of barrier protection, like a condom)
- Avoid douching (it can cause vaginal flora changes)
- Avoid using spermicidal jellies (they can upset vaginal flora)
- Eat foods rich in probiotics, or take high-quality probiotics
- Wear loose-fitting cotton clothing (particularly your knickers)
- Clean your vulva with warm water only (your vagina is a self-cleaning machine, don’t you ever forget it)
How to treat a vaginal yeast infection?
To treat yeast infections, there are several over-the-counter antifungal medications available as a first line of defence. OTC antifungal creams are available in one, three, and seven-day doses.
One-day over-the-counter antifungal creams have the strongest concentration, with the three-day treatment having a lower concentration and the seven-day treatment being the weakest concentration. It won’t matter which course of antifungal cream treatment you choose, the healing time remains the same.
Symptoms of a yeast infection should clear within a week or two, depending on the state of your immune system and the severity of symptoms. If symptoms haven’t cleared within seven days, you should see a doctor for prescription strength antifungal cream or medications. Even if symptoms subside and you begin to feel better, make sure to always complete a full course of treatment to prevent recurrent yeast infections from occurring.
In the event of frequent yeast infections, your doctor may suggest a maintenance program incorporating oral or vaginal antifungal medications.
If birth control pills are the cause of your yeast infection, your doctor may prescribe a low-dose oral contraceptive, like the vaginal ring, that has lower hormone levels in comparison to oral contraceptives. If you’re experiencing chronic yeast infections, your doctor may recommend stopping hormonal birth control and starting one of the other types of contraception available in Australia.
For asymptomatic cases of thrush and BV, your doctor will be in a position to recommend the appropriate treatment. Avoiding sex, tampons, and other period products during a yeast infection will also assist in speeding up the recovery time (keep in mind that these practices are likely to be uncomfortable during a yeast infection, so you probably won’t be inclined to do them anyway).
When to see a doctor?
As a general guide, if you still have symptoms after seven days of using OTC medication, visit your doctor, as you may need a prescription-strength antifungal cream or oral fluconazole to help in clearing the infection.
You should also visit your doctor if you have abdominal pain, fever, diabetes, HIV, or a change in vaginal discharge accompanied by a strong, unpleasant odour.
Want hassle-free healthcare?
Yeast infections are extremely common, so there’s no need to be embarrassed or worried if you think you have one. The good news is that once-off and chronic yeast infections are easily treated with over-the-counter treatments and prescription medication.