When it comes to contraception, there is a multitude of options available. The intrauterine device (IUD) is one of the most effective and hassle-free choices. In this guide, we delve into the world of IUDs, exploring what they are, how they work, the different types available, their benefits, potential side effects, and more. Whether you’re considering this birth control method or simply curious about it, our guide will provide you with all the essential information you need to make an informed decision.
What is an IUD and How Does it Work?
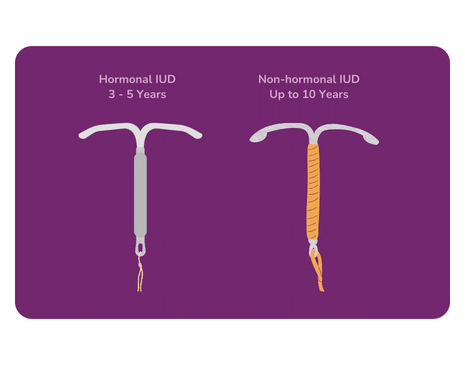
An intrauterine device (IUD) is a highly effective, long-term birth control method that is inserted into the uterus to prevent pregnancy. This T-shaped device comes in two main types: hormonal and non-hormonal, and it works by altering the environment of the uterus to make it less hospitable for sperm and implantation of a fertilised egg.
The non-hormonal IUD, typically made of copper, releases copper ions that are toxic to sperm, impairing their ability to reach and fertilise an egg. On the other hand, hormonal IUDs release a small amount of progestin, a synthetic hormone, which thickens cervical mucus, making it difficult for sperm to pass through and also alters the uterine lining, preventing implantation.
How Long Does an IUD Last?
After someone has an IUD inserted, the duration depends on the specific type and brand of IUD chosen. Hormonal IUDs can provide contraception for up to 3 to 5 years. Non-hormonal IUDs can last for up to 10 years.
It’s important to note that the actual duration an IUD remains effective may vary slightly based on individual factors and the specific brand. Some healthcare providers may also recommend replacing an IUD before its maximum lifespan to ensure continued effectiveness.
When the IUD’s effectiveness period is nearing its end, discuss with your healthcare provider whether to have it removed and replaced or consider alternative birth control methods if you wish to continue contraception.
Ultimately, the choice of the IUD’s lifespan should align with your family planning goals and the contraceptive method that best suits your needs and preferences. Your healthcare provider can guide you in selecting the most appropriate IUD based on your circumstances.
The Benefits of an IUD: Exploring its Effectiveness
The intrauterine device (IUD) is gaining popularity as a highly effective and hassle-free birth control method, and its benefits extend far beyond just contraception.
Exceptional Effectiveness
One of the standout benefits of IUDs is their remarkable effectiveness in preventing pregnancy. Both hormonal and non-hormonal IUDs are over 99% effective, making them one of the most reliable contraception options available—this rivals the efficacy of the contraceptive pill and permanent sterilisation methods.
Long-Lasting
IUDs offer a long-lasting contraceptive solution. Depending on the type and brand, they can provide protection for up to a decade, reducing the need for frequent contraceptive management.
Set-and-Forget Convenience
Once someone has an IUD inserted by a healthcare provider, there’s no need for daily, weekly, or monthly maintenance. You don’t have to remember to take a pill (we all know what happens when you miss a birth control pill) or use a barrier method before sexual activity. This “set-and-forget” convenience is a significant advantage, especially for those with busy lifestyles.
Rapid Reversibility
If you decide to conceive in the future, IUD removal typically allows for a quick return to fertility. Unlike other contraceptive methods, the reversibility of IUDs is almost immediate, giving you control over your family planning.
Highly Discreet
IUDs are a discreet form of contraception. Once inserted, they remain hidden inside the uterus, so there are no visible or palpable reminders of contraception.
Lower Hormone Dosage
Hormonal IUDs release a minimal amount of progestin locally, directly into the uterus. This results in fewer hormonal side effects than other methods, such as birth control pills.
Menstrual Benefits
Some hormonal IUDs can lead to a lighter menstrual cycle or even the absence of menstruation for some individuals. This can be a welcome benefit for those who experience painful or heavy periods.
Reduced Cramping
Non-hormonal copper IUDs, while known for potentially causing heavier periods, are associated with reduced cramping for some users. Psst – learn more about painful period cramps.
Cost-Effective
Over the long term, IUDs can be cost-effective compared to other birth control methods. Although the initial insertion cost may be relatively high, their extended lifespan makes them a budget-friendly option.
Privacy and Autonomy
With an IUD, you have a high level of control over your reproductive choices. You can decide when to start or expand your family without the need for immediate medical intervention.

Hormonal vs. Copper IUD: Which is Right for You?
Choosing the right intrauterine device can be a pivotal decision for your reproductive health. IUDs come in two primary categories, each with unique advantages and considerations.
Hormonal IUD
Contraceptive Efficacy: Hormonal IUDs are highly effective, offering over 99% protection against pregnancy. They release a steady, low dose of a synthetic hormone into the uterus, primarily affecting cervical mucus and the uterine lining to prevent fertilisation and implantation.
Reduced Menstrual Discomfort: Many women who use a hormonal IUD experience lighter periods and reduced menstrual cramping. In some cases, menstruation may even stop altogether, providing a welcome relief for individuals with heavy or painful periods.
Longevity: The hormonal IUD provides effective contraception for up to several years, depending on the specific type. Their longevity means less frequent interventions for birth control.
Hormonal Considerations: While the hormonal dose is minimal and localised, some individuals may still experience hormonal side effects, such as mood changes (similar to mood changes on the pill), breast tenderness, or irregular bleeding. If you are sensitive to hormonal changes, a copper IUD might be a more suitable option.
Copper IUD
Non-Hormonal: The copper IUD is a non-hormonal method of contraception. It works by releasing copper ions, which are toxic to sperm, preventing fertilisation. This makes it a suitable choice for those who prefer a hormone-free birth control method.
Longest Lasting: Copper IUDs have the longest lifespan among IUDs, with some options providing protection for up to a decade. If you desire an extended contraceptive solution without hormonal influences, the copper IUD may be the right choice for you.
Heavier Periods: A potential drawback of copper IUDs is an increase in menstrual flow and cramping for some users. This can be challenging for individuals who already experience heavy or painful periods.
Non-Hormonal Benefits: If you prefer to avoid hormonal influences on your body, the copper IUD offers effective contraception without introducing synthetic hormones. This is a significant advantage for individuals seeking hormone-free options.
Who Should Not Use an IUD?
While Intrauterine Devices (IUDs) are a highly effective and widely used form of contraception, there are certain circumstances in which individuals should not use an IUD. It’s essential to consult with a healthcare provider for personalised advice, but here are some common situations where IUDs may not be suitable:
Pregnancy: IUDs should not be inserted if you are already pregnant, as they are designed for contraception, not termination of pregnancy.
Certain Uterine Conditions: Conditions such as an abnormally shaped uterus, uterine fibroids that distort the uterine cavity, or a recent uterine infection may make IUD insertion problematic or less effective.
History of Pelvic Inflammatory Disease (PID): If you have had PID in the past, using an IUD may increase the risk of recurrent PID, which can lead to serious health complications.
Active Sexually Transmitted Infection (STI): If you currently have an active STI, particularly chlamydia or gonorrhea, it’s generally advisable to treat the infection before considering IUD insertion to prevent complications.
Unexplained Vaginal Bleeding: If you experience unexplained vaginal bleeding, it’s important to investigate the cause before considering IUD insertion.
Severe Menstrual Disorders: In cases of extremely heavy menstrual bleeding or severe menstrual cramps, a healthcare provider may recommend alternative treatment options or IUD types, so it’s important to discuss your specific situation.
Prior IUD Complications: If you’ve previously had complications or issues with an IUD, it may not be the best choice for you.
It’s crucial to consult with a healthcare provider who can assess your individual medical history, conduct a thorough evaluation, and provide guidance on whether an IUD is a suitable contraceptive option for you. The decision should be made with careful consideration of your unique circumstances, health, and contraceptive preferences.
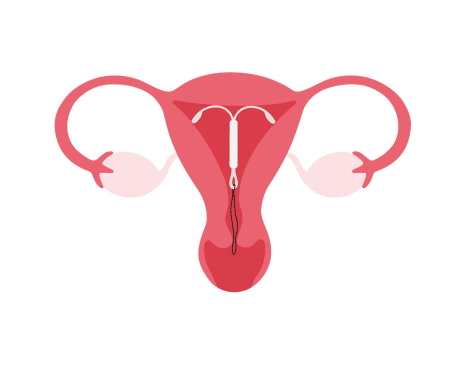
Where is the IUD Placed, and How Does it Work?
The IUD is a small, T-shaped contraceptive device that is inserted into the uterus by a healthcare provider. The placement of the IUD and its mechanism of action can be summarised as follows:
Placement
Medical Setting: IUD insertion is typically performed in a medical setting by a trained healthcare provider (doctor or nurse), such as a doctor’s office or a clinic.
Positioning: The healthcare provider will have you lie on an examination table, similar to a pelvic exam. They will insert a speculum into the vagina to gain access to the cervix.
Cervical Measurement: Before insertion, the provider will measure the length of your cervix to ensure that the IUD is placed in the correct position within the uterus.
IUD Insertion: The IUD is inserted through the cervix and into the uterine cavity using a thin, flexible applicator. Once in place, the provider releases the IUD, allowing it to unfold and settle within the uterus.
String Trimming: After the IUD is positioned, the provider trims the strings attached to the device, leaving a short string outside the cervix. These strings are used for periodic checks and for removal when necessary.
Mechanism of Action
Hormonal IUDs release a small, steady dose of a synthetic hormone progestin into the uterine cavity. This hormone thickens cervical mucus, making it difficult for sperm to pass through, and it also changes the uterine lining, making it less receptive to implantation. The progestin may also inhibit ovulation in some cases, though this is not the primary mechanism of action.
Copper IUDs do not contain hormones. Instead, they have copper wire wrapped around the stem of the device. Copper ions are released into the uterus, creating an environment that is toxic to sperm. This impairs the sperm’s ability to swim and fertilise an egg.
The IUD’s placement and mode of action ensure that it remains highly effective in preventing pregnancy. Once inserted, it offers long-term, low-maintenance contraception. The strings left outside the cervix allow for easy monitoring by you and your healthcare provider to ensure the IUD is in the correct position.
Understanding the Different Types of IUDs
Intrauterine devices can be categorised into two main types, each offering distinct characteristics. Hormonal IUDs prevent pregnancy by releasing a synthetic hormone into the uterine cavity, providing highly effective contraception for several years. On the other hand, copper IUDs are hormone-free and prevent pregnancy by releasing copper ions, making the uterine environment inhospitable to sperm. These non-hormonal devices typically offer extended protection.
When deciding between the two types of IUDs, it’s essential to consider factors such as your health, contraceptive preferences, and the duration of contraception needed. Consulting with a healthcare provider can help you choose the IUD that best aligns with your unique circumstances and family planning goals.









